Promoting healthy behaviors has become part of the lexicon of healthcare in recent months, and that is due to several forces converging. The Centers for Medicare and Medicaid Services (CMS) has taken the lead in changing the way that healthcare services are provided and reimbursed, and this has been an initiative that has been underway for at least the last four years.
Value-Based Care
Both Seema Verma, the CMS Administrator, and Adam Boehler, the Director of the Centers for Medicare and Medicaid Innovation, have been outspoken regarding the need to address proactively keeping people healthy, instead of waiting until they get sick and require expensive services. This represents a significant change to the US healthcare system, and is known as value-based care.
In value-based care, providers are rewarded for the relative health of their patients, instead of getting paid to treat them when they are ill. The management of chronic conditions is a key to lowering healthcare costs and improving patient outcomes.
What’s the Cost?
60% of all Americans have at least one chronic condition, and 40% have two or more.
The U.S. Centers for Disease Control and Prevention (CDC) says that chronic diseases such as heart disease, cancer, and diabetes are the leading causes of death and disability in the United States. They are also leading drivers of the nation’s $3.3 trillion in annual health care costs. The CDC goes on to estimate that eliminating three risk factors – poor diet, inactivity, and smoking – would prevent: 80% of heart disease and stroke; 80% of type 2 diabetes; and, 40% of cancer.

The Need for Incentives
The interesting twist is that when asked, US consumers state that they want more rewards for healthy living from their health insurance companies. 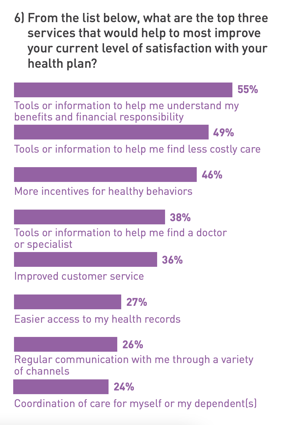 In a survey of 3000 consumers conducted by HealthEdge in 2021, the question was asked: What are the top three (3) services that would help to most improve your current level of satisfaction with your health plan? The results across the entire survey group were clear – the third most popular response, with 46%, was “More incentives for healthy behaviors.”
In a survey of 3000 consumers conducted by HealthEdge in 2021, the question was asked: What are the top three (3) services that would help to most improve your current level of satisfaction with your health plan? The results across the entire survey group were clear – the third most popular response, with 46%, was “More incentives for healthy behaviors.”
Perhaps the most startling result came from Millennials, who now make up the largest age cohort in the U.S. and will soon have the buying power commensurate with their numbers. 53% of Millennials want more incentives for healthy behaviors from their health plan, and 44% stated that those health incentives are missing and impacting their satisfaction with their health plan. This is a cohort that must be addressed.

How Employers Can Help
Health plans are not alone in the opportunity to exert direct and significant influence on consumers. Employers can have a fundamental role in impacting health and well-being. In a recent 2021 study conducted by Aflac, 77% of employees say it is extremely or very important that their benefits providers show they care about them – higher for the younger generations - 87% for millennials and 84% for Gen Z.
Interestingly enough, 72% of employers think employees understand total health care costs well. However, just 59% of employees say they actually do.
These are just a couple of many findings in the summary of current benefit trends. A comprehensive and holistic wellness program will help employees change their lifestyle and make better choices, resulting in higher productivity and job satisfaction.

The same report finds that Millennials, more than any other group, factor in benefits like health and wellness programs in deciding whether to take or remain in a job. This is consistent with the HealthEdge survey on desired benefits from health plans.
And among those healthy incentive programs, it has been proven that cash rewards do not have a sustained impact on life habits. Incentives such as gift cards for healthy habits make a long-lasting difference, helping to contain costs of healthcare, improve overall health outcomes and boost employee engagement all at the same time.
A special thank-you to our guest Health & Wellness writer Harry Merkin of HealthEdge.












.png?width=600&height=600&name=3D8DC522-2245-490E-AA26-63567A199A4C%20.png)